Texas Heroes on the Frontlines

Nurse Lena Thixton, Dr. Otto Marquez, and Chaplain Nancy Parsons
Photos by Kim Leeson~
The waiting areas of emergency rooms are empty, these days. Masks and layers of protective equipment hide all but the eyes of professionals and of patients who’ve come in because of a broken arm, a stroke, or the monster virus that has wrought the changes in protocol and normalcy. Family members hear updates on loved ones’ conditions only through phone calls or computer screens.
COVID-19 may have turned the world upside-down, but highly trained hospital staffs around the world refuse to let the pandemic steal their souls — or their collective resolve to keep fighting.
At Texas Health Presbyterian Hospital Dallas, we caught up with a trio of such dedicated professionals. They are only three of the hundreds who put their own lives on the line every day.
Here is what Dr. Otto J. Marquez; Lena Thixton, RN; and Chaplain Nancy Parsons face at work, how this experience has changed them all, and where they each find the strength to keep going.
 Dr. Otto J. Marquez
Dr. Otto J. Marquez
Dr. Otto J. Marquez, an attending emergency room physician, likens the COVID-19 vaccine to wearing a bulletproof vest at work. And, while he knows that nothing is 100% effective in fighting this or any virus, getting the vaccine provided a gift of protection — a shot of hope into his spirit as well as medicine into his arm.
“When I got it at the hospital, there was a long line and it felt like something historic, like the polio vaccine,” Dr. Marquez said.
“After the first shot and especially after the second, I was so excited. I was so happy.”
It’s been a long past 12 months for Dr. Marquez and his colleagues. “COVID has definitely influenced our lives,” Dr. Marquez, a 27-year veteran of the ER, said. “I take [the virus] very seriously: Treat everyone like they have COVID until proven otherwise. That’s what you need to do.”
Even without a pandemic, emergency room work is tough. It is alternately unrelenting and rewarding, invigorating and exhausting.
“Some days are really crazy,” he said. “We have to intubate two, three people. We’re running around; the place is packed. I just try to take care of people. We all tend to think of COVID and not of everything else that’s happening.
But people are still having heart attacks; they’re still having strokes.”
Dr. Marquez added: “Manage chaos, that’s what we do. Manage craziness.” In this carefully choreographed chaos, the musical soundtrack is one of questions and answers; of beeps and heart beats; of hurried footsteps and purposeful breaths. Counting on each other has always been the norm, and Dr. Marquez said the pandemic has served to deepen that bond.
“This has brought me closer to my colleagues, absolutely,” he said. “We’re like soldiers going to work every day. It’s us against this virus. The ER is a team effort, a team sport. We’re working together. We all need each other; we could never work without any of them. That’s the most important thing.”
That became especially apparent when a beloved colleague almost died from the virus early in the pandemic. The Dallas Morning News wrote about the roles which almost 100 people, including Dr. Marquez, played in saving Dr. Charles Iliya’s life.
“It was very scary,” Dr. Marquez said. That experience heightened an awareness we all know in our heads, but that the pandemic has brought into heartfelt focus: Any day, at any moment, life can change.
“You could get something at work and be dead in two weeks,” he said. “I’ve never had to deal with that.” Now he does. And while he has always been empathetic when patients pass away, he said, he is even more so now.
“I make a lot more phone calls because the family can’t be in the room,” Dr. Marquez said. “They can’t see their loved ones as they’re dying. They can’t always have funerals.”
He said he’s learned not to be wary and pessimistic but “to enjoy the day, to be positive and be happy. And I am. I have a better perspective about everything.”
He’s always cherished time with his wife, Kim. Now, he does so even more. They live near White Rock Lake, where they enjoy walking together. But they don’t talk about work, which, he said, he has learned to compartmentalize.
He’s always loved going to the gym, but when he returned recently — after almost a year’s absence — people tended to take their masks off while working out.
“I don’t want to be Mr. Grandpa, walking around asking people to cover their faces,” Dr. Marquez said.
And he gets frustrated seeing maskless people in public, but “what can you do?” he said.
Save lives, in his case. Be grateful. Appreciate even more every breath, step, and chance to make a difference.
To stop, he said, “and smell the roses more.”
 Nurse Lena Thixton
Nurse Lena Thixton
Lena Thixton, a Texas Health emergency room nurse, hasn’t seen her patients’ faces in a year. Nor have they seen hers.
But masks and layers of lifesaving protective equipment will never diminish the power of human contact. So Thixton still touches the shoulders of those in her care and she still reaches for their hands.
Because despite all the changes that COVID-19 and its protocols have necessitated, three aspects of her job hold steady: The commitment to patients, the belief in the work she calls her passion, and the knowledge that everyone she works with has her back as much as she has theirs — more now, if that’s even possible, than ever before.
“I don’t have that stress of being alone, because you’re never alone,” Thixton said. She started working at the hospital when she was in nursing school 11 years ago and has worked in the ER for four years. “If you ever need help, there’s always help.”

Additionally, long before COVID-19 became part of the world’s lexicon and upended everyone’s life, Texas Health — having dealt with the Ebola virus in 2014 — was prepared.
“We had equipment. We’d been trained for SARS, MERS, tuberculosis,” Thixton said. “We were trained on how to wear isolation equipment. When COVID happened, it was all very familiar.”

When patients leave the ER for continued care in the hospital, Thixton said she and her colleagues “have kind of perfected this routine so we don’t spread the virus. If they’re stable, we’ll have someone transport them to a room.
If they’re unstable, we’ll have two nurses. One is the ‘clean’ person who touches the elevator buttons and doors.
Only the ‘contaminated’ person touches the patient and the bed.”
Such knowledge and camaraderie have been comforting, especially in a profession and at a time when the stress level is incredibly high and every day is difficult. Thixton’s shifts start at 7 a.m. and runs until 7 p.m. More often than not, she stays even later.
“I don’t like to leave tasks undone,” Thixton said, “so I make sure, if a patient needs blood drawn or an IV, that the nurse coming on doesn’t have to deal with a lot of stress right off the bat. I’ll stay a little late to help nurses and they’ll do the same.”
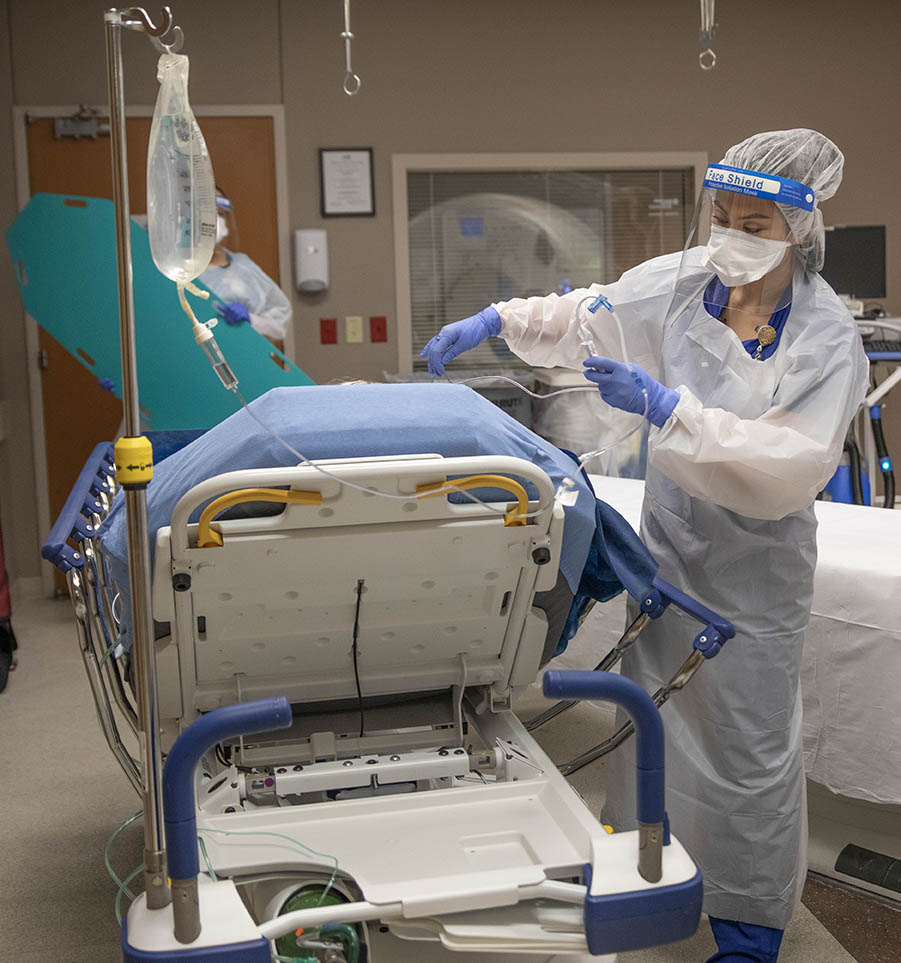
Thixton is always on the go. Sometimes hours will pass before she realizes she hasn’t had time to eat or go to the bathroom.She said the toughest part has been keeping family members informed when they can’t be at their loved one’s bedside.
These days, Thixton can look into their eyes only through a computer screen and talk to them only through a phone call.
She is their lifeline to their loved ones, a responsibility she takes very seriously. “Not knowing the status of their loved ones adds unnecessary stress to an already difficult situation,” she said.
This has, without a doubt, been a year of struggles, sadness, and uncertainty. And yet, for Thixton, it’s also been one of newfound strength.
“I don’t want to sound cheesy, but this has made me a better nurse,” Thixton said. She de-stresses with kickboxing and weight training. “Little challenges I’d stress over before, now I’m thinking, ‘I handle COVID; this is nothing. I can do it.’”
And she continues to ask the same two questions she’s always asked herself driving home from the hospital: Did I make a difference in my patients’ care? Did I improve their lives? “That helps me unwind and go home,” Thixton said, “knowing I made a difference.”
 Chaplain Nancy Parsons
Chaplain Nancy Parsons
As a hospital chaplain, Nancy Parsons spends time with people of all spiritual backgrounds. She has done this for nearly 24 years; she’s been trained extensively and continues to learn. Every day is different, and every conversation is unique.
But she can narrow what she does down to one word: Listen.
Even when layers of protective gear keep her from seeing those with whom she spends precious time. Even when COVID protocol keeps her from entering a patient’s room to ask if there’s anything she can do. She listens.
“I find sometimes it’s not what you say but the fact that you are there,” she said. “We so undervalue what listening does for another person.”
At the beginning of the pandemic, when the hospital was shut down to all but employees and patients, she did that listening via tele-chaplaincy.
“Instead of being at the bedside with a family member, we’d be on the phone,” Parsons said. “I’d be doing my assessment of what emotions they’re going through, their feelings, thoughts, what the context of the loved one’s life is, what the relationship is.”
She has honed those skills every day she has been a chaplain. But at first, she said, “the pandemic made me go back through and visit some of them of those on a deeper level.”
When medical personnel are working with patients, they’re going through a concrete checklist. Her focus is more ethereal, more tangible.
“There are certain things I’m listening for which are a part of the process of helping,” Parsons said. “We all have a narrative of our life: We have a past story, a present story, and we have a future story. How do we tell it in such a way that it gives meaning and purpose, that it talks about things we value, things we believe in?”

Those often heart-wrenching conversations happen any hour of the day or night. Sometimes they’re with individuals, while other times she’s part of family meetings. The latter often involve the pain of knowing a loved one will not get better. How, then, will the family go on? What is their future story?
“We try to get them to draw on spiritual resources, their strengths,” she said. “A lot of times that means acknowledging a struggle.” Her work includes being there for hospital staff, too. She supports them, prays with them, listens to them.
“A lot of medical people are like, ‘I have to be strong; I can’t show my emotions,’” she said. “But we’re trying to get them to tell their story, too. For a lot of them, it’s just being with them in the battle.”
What keeps her going is her stalwart belief that, as human beings, we are all about connection. On days that are particularly heavy, Parsons said she relies first on her faith, “knowing the spirit that unites us, the spirit God has put within us, sustains me.”
She makes sure to get a lot of sleep, to eat healthy foods, and to exercise (wearing three masks when she goes to the gym).
“God has put God’s self, God’s spirit, within all of us,” Parsons said. “I have people I work with who are Hindi. They acknowledge my belief system, and I, theirs; that we need each other to do this and that we’re not alone. God promised to walk with us. God promises to be with us.”

 Dr. Otto J. Marquez
Dr. Otto J. Marquez Nurse Lena Thixton
Nurse Lena Thixton Chaplain Nancy Parsons
Chaplain Nancy Parsons



